The Role of Rotary Chair Testing in Comprehensive Vestibular Assessment: Principles and Clinical Applications
Introduction
Dizziness, vertigo, and balance disorders are among the most frequent clinical complaints in neurology and otolaryngology. However, identifying the precise origin of vestibular dysfunction often requires objective measures beyond bedside observation. In modern vestibular diagnostics, the rotary chair remains a cornerstone technology. By providing precise, computer-controlled rotational stimuli, it allows clinicians to quantify the vestibulo-ocular reflex (VOR) under highly repeatable conditions.
While newer technologies like the Video Head Impulse Test (vHIT) have expanded the diagnostic toolkit, rotary chair testing maintains a unique and essential role. It is particularly valued for its ability to assess the low- to mid-frequency range of the rotational VOR (rVOR) and serves as the clinical "gold standard" for identifying bilateral vestibular weakness.
Technical Foundations: How the Rotary Chair Measures Vestibular Function
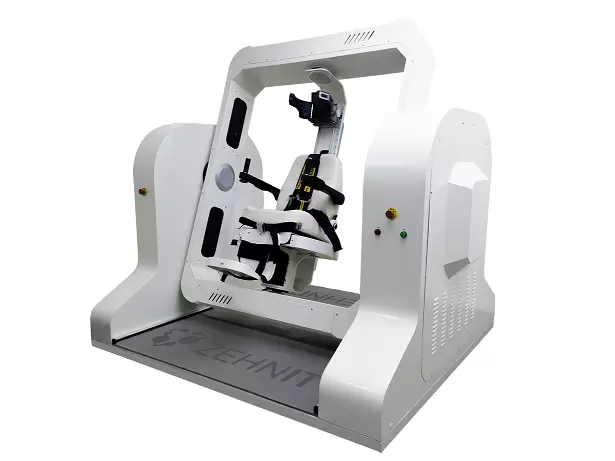
The primary objective of rotary chair testing is to evaluate the horizontal semicircular canals and their associated neural pathways. During a test, the patient is seated in a precision motorized chair that rotates around a vertical axis. As the chair moves, the vestibular system detects angular acceleration and triggers compensatory eye movements—known as nystagmus—to maintain gaze stability.
Advanced systems, such as modern digital rotary chair platforms, integrate high-speed infrared VNG (videonystagmography) goggles to record these eye movements in total darkness. The system supports comprehensive rotary chair testing, including standard paradigms such as Sinusoidal Harmonic Acceleration (SHA) and Velocity Step Testing (VST), and then the software calculates four primary parameters:
•Gain: The ratio of eye velocity to chair velocity, indicating the overall responsiveness of the vestibular system.
•Phase: The timing relationship between head movement and eye movement, which helps locate the site of a lesion.
•Symmetry: A comparison of responses during clockwise versus counter-clockwise rotation, used to identify unilateral deficits.
•Time Constant: The rate at which eye velocity decays after rotation stops. It mainly represents central velocity storage function but is also influenced by peripheral vestibular input, with reduced values seen in vestibular hypofunction.
Core Clinical Protocols
Sinusoidal Harmonic Acceleration (SHA)
Sinusoidal Harmonic Acceleration is the most commonly performed rotary chair protocol. In this test, the chair moves in a smooth sinusoidal pattern across a range of frequencies, allowing the clinician to observe how vestibular responses change as the stimulus becomes slower or faster. Rotary chair testing is commonly described as a low- to mid-frequency vestibular test, often covering approximately 0.01 to 0.64 Hz depending on the system and protocol.
SHA is especially useful because it provides a dynamic view of vestibular performance rather than a single-point measurement. It helps clinicians assess how the rotational VOR behaves under conditions that are more physiologically representative than very low-frequency stimulation alone.
Velocity Step Test
The Velocity Step Test uses a rapid acceleration to a constant chair velocity, followed by observation of the induced nystagmus and its decay over time. Its main clinical value lies in analyzing post-rotatory response dynamics, especially the time constant. This can provide useful information when clinicians want to better understand vestibular responsiveness and central velocity-storage behavior.
The Diagnostic Value: Why Rotary Chair Testing Remains Essential
Despite the prevalence of caloric testing and vHIT, the rotary chair offers distinct clinical advantages that make it indispensable for specialized balance centers.
Important Role in Assessment of Bilateral Vestibular Weakness
Rotatory chair testing is widely regarded as the criterion standard for evaluating bilateral vestibular weakness. This is one of its most important clinical roles. Bilateral vestibular loss may be difficult to characterize because the deficit can be relatively symmetric, and the patient may present with chronic imbalance or oscillopsia rather than dramatic side-to-side asymmetry. Rotary chair testing helps quantify residual rotational vestibular function under controlled conditions and is therefore particularly valuable in this setting.
Monitoring Compensation and Change Over Time
Because the chair can deliver the same stimulus parameters across repeated visits, it is also useful for monitoring vestibular compensation, disease evolution, or response to therapy. This repeatability is one of the reasons rotary chair testing remains relevant in modern neurotology and vestibular practice.
Improved Patient Comfort
Compared with caloric testing, which requires thermal stimulation of the ear canal with water or air and may provoke marked discomfort or nausea, rotary chair testing is generally better tolerated by many patients, including children and individuals with middle ear pathologies.
Expanded Capabilities: Beyond Standard Rotation
For a standard rotary chair, the core focus is rotational VOR testing. However, advanced chair platforms can offer a broader clinical scope, which is highly relevant for institutions aiming to build a more capable vestibular service.
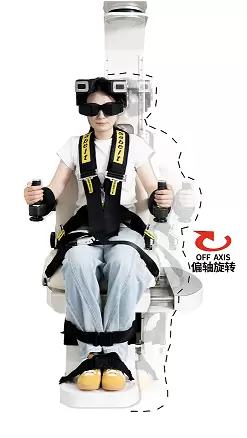
Eccentric or Off-Axis Testing
Some rotary chair systems support off-axis centripetal acceleration or related eccentric protocols. These allow dynamic assessment of otolith-related function, including applications such as dynamic subjective visual vertical (SVV) testing. This expands the chair’s role from conventional semicircular canal assessment toward more advanced vestibular investigation.
Chair-Based BPPV Diagnosis and Treatment
Another meaningful platform advantage is the ability to support BPPV diagnosis and treatment. Repositioning chairs and mechanical rotational chairs have been used to assist positional testing and therapeutic maneuvers, particularly in patients who are difficult to examine manually because of age, obesity, limited mobility, neck or back problems, anxiety, or poor tolerance of repeated head-and-body repositioning.

VVOR and VORS Assessment
Advanced rotary chair systems can also support assessment of visually enhanced vestibulo-ocular reflex (VVOR) and vestibulo-ocular reflex suppression (VORS). These paradigms evaluate the interaction between visual and vestibular inputs by requiring patients to either enhance or suppress vestibular-driven eye movements under visual conditions. The ability to precisely and flexibly control rotational frequency allows for targeted assessment across different stimulus conditions. VVOR reflects the combined contribution of visual tracking and vestibular function, whereas VORS assesses the ability to suppress the VOR, a process largely mediated by central mechanisms, particularly the cerebellum. This expands the clinical utility of the rotary chair beyond peripheral assessment, providing valuable insight into central vestibular disorders and visual–vestibular integration deficits.
Motion Sickness Assessment and Rehabilitation
Rotary chair platforms can also be applied in the assessment and management of motion sensitivity. Controlled rotational stimuli can be used to evaluate susceptibility to motion sickness, which is closely related to the dynamics of the velocity storage mechanism and sensory conflict processing. In addition to diagnostic use, these systems can support habituation-based rehabilitation, where repeated exposure to motion stimuli reduces symptom severity over time. This further extends the role of the rotary chair from diagnostic testing to an active tool in vestibular rehabilitation for patients with motion intolerance or chronic dizziness.

Future Directions: AI and Data Integration
The most credible future developments in rotary chair technology are likely to center on software intelligence, connectivity, and data analysis.
AI-Assisted Eye Movement Analysis
Recent developments in vestibular diagnostics indicate increasing interest in AI-based eye movement analysis. Machine learning methods are being explored to help identify nystagmus patterns, support automated interpretation, and improve diagnostic consistency. For rotary chair systems, this trend points toward more efficient review of complex motion-response datasets and stronger clinical decision support.
Cloud-Enabled Review and Data Management
Another practical direction is cloud-enabled storage, review, and collaboration. As vestibular testing generates larger and more information-rich eye-movement datasets, secure cloud-based platforms may improve documentation, remote specialist review, and multi-site clinical collaboration.
Conclusion
The rotary chair is more than a traditional diagnostic tool; it is a sophisticated platform for quantitative vestibular analysis. By bridging the gap between low-frequency caloric tests and high-frequency vHIT, it ensures a comprehensive evaluation of the balance system. As technology continues to integrate AI and multi-axial motion, the rotary chair will remain a vital component in the accurate diagnosis and long-term management of patients with vestibular disorders.