What Is Computerized Dynamic Posturography (CDP)? A Complete Guide to Balance Assessment
Maintaining balance is a complex physiological process that depends on the integration of multiple sensory systems, including visual input, vestibular signals from the inner ear, and proprioceptive feedback from muscles and joints. When these systems become impaired or poorly coordinated, individuals may experience dizziness, instability, or an increased risk of falls.
Computerized Dynamic Posturography (CDP) is a specialized clinical method, often referred to as a CDP balance test, used to objectively evaluate how the body maintains balance under controlled sensory conditions. By selectively altering visual cues and support surface stability, CDP helps clinicians analyze how patients use visual, vestibular, and somatosensory information to maintain posture.
This guide explains the principles, procedures, and clinical applications of Computerized Dynamic Posturography (CDP), providing a comprehensive overview of how the technology supports modern balance assessment.
Understanding Balance and Postural Control
Human balance depends on the coordinated function of three major sensory systems:
1.Visual System
Provides information about body orientation relative to the surrounding environment.
2.Vestibular System
Located in the inner ear, it detects head movement and spatial orientation relative to gravity.
3.Somatosensory System
Includes proprioceptive signals from muscles, joints, and the feet that inform the brain about body position.
The central nervous system continuously integrates these signals to maintain postural stability. When one sensory system becomes unreliable, the brain adjusts the relative weighting of sensory inputs to maintain balance.
Disruption in this integration process—due to vestibular disorders, neurological disease, or musculoskeletal problems—can result in impaired balance.
What Is Computerized Dynamic Posturography (CDP)?
Computerized Dynamic Posturography (CDP) is an objective diagnostic technique used to evaluate balance control and sensory integration by measuring how the body responds to controlled perturbations in visual and support surface conditions.
Unlike simple bedside balance tests, CDP quantifies postural stability by measuring center-of-pressure (COP) displacement and postural sway while different sensory inputs are manipulated. This allows clinicians to determine how effectively a patient relies on visual, vestibular, or somatosensory information when maintaining posture.
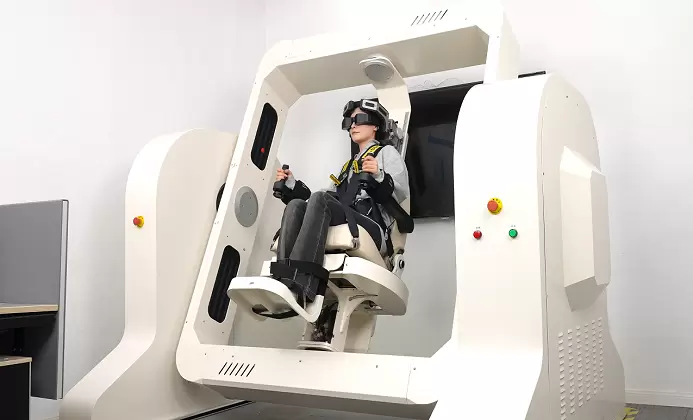
A typical CDP balance assessment system includes:
•A force platform that measures center-of-pressure movement
•A movable support surface that can alter somatosensory feedback
•A visual surround or immersive visual environment that modifies visual input
•Analytical software that processes sway data and generates clinical reports
Rather than identifying a single anatomical lesion, CDP provides a functional evaluation of postural control, helping clinicians understand patterns of sensory dependence and balance impairment.
Sway-Referenced Visual Surround Technology: Mechanical Systems and VR-Based Environments
In traditional CDP systems, the visual surround is implemented as a movable enclosure that shifts in relation to the patient’s body sway, creating controlled visual conflicts that challenge visual dependence during balance testing. This sway-referenced visual surround remains a key component of classic Sensory Organization Test protocols.
In recent years, technological advances have introduced virtual reality (VR)–based visual environments, which can generate immersive visual motion or simulated environments through digital displays or head-mounted devices. These VR stimuli allow clinicians to design more flexible testing scenarios and rehabilitation tasks.
However, some patients may experience discomfort, motion sensitivity, or reduced tolerance to immersive VR environments, which can potentially influence test performance or patient compliance. For this reason, systems that combine both traditional mechanical visual surrounds and VR-based visual stimuli offer greater clinical flexibility, allowing clinicians to select the most appropriate visual condition based on patient tolerance and testing objectives.
Modern platforms such as the VertiPlatform™ – Dynamic integrate both approaches within a single device, enabling clinicians to switch between conventional visual surround testing and VR-based environments to support reliable balance assessment across different patient populations.
Key Components of CDP Testing
Sensory Organization Test (SOT)
The Sensory Organization Test (SOT) is one of the core protocols used in computerized dynamic posturography systems. It evaluates how effectively patients use different sensory inputs for maintaining stability.
The test includes six standardized conditions:
1.Fixed support surface, eyes open – all sensory inputs available
2.Fixed support surface, eyes closed – visual input removed
3.Fixed surface with sway-referenced visual surround – visual information becomes unreliable
4.Sway-referenced support surface, eyes open – somatosensory input becomes unreliable
5.Sway-referenced support surface, eyes closed – reliance primarily on vestibular input
6.Sway-referenced surface and visual surround – both visual and somatosensory cues become unreliable
By analyzing postural sway across these conditions, clinicians can determine how patients rely on different sensory systems for balance.

Motor Control Test (MCT)
The Motor Control Test evaluates the automatic postural responses triggered when the support surface suddenly moves.
The platform performs brief forward or backward translations while the system measures:
•Reaction time
•Response strength
•Symmetry between lower limbs
This test assesses the integrity of automatic balance responses and neuromuscular coordination.

Adaptation Test (ADT)
The Adaptation Test (ADT) evaluates how well patients adjust to repeated surface perturbations.
The platform tilts upward or downward in a series of trials, and the system measures how quickly the patient adapts by minimizing sway. This test provides insight into adaptive motor control mechanisms.
In addition to core CDP protocols such as SOT, MCT, and ADT, many modern CDP systems can also perform other instrumented balance assessments, including Romberg testing, the modified Clinical Test of Sensory Interaction on Balance (mCTSIB), Limits of Stability (LOS), and Rhythmic Weight Shift (RWS), providing a broader evaluation of postural control.

How CDP Is Performed
A typical Computerized Dynamic Posturography assessment follows several steps.
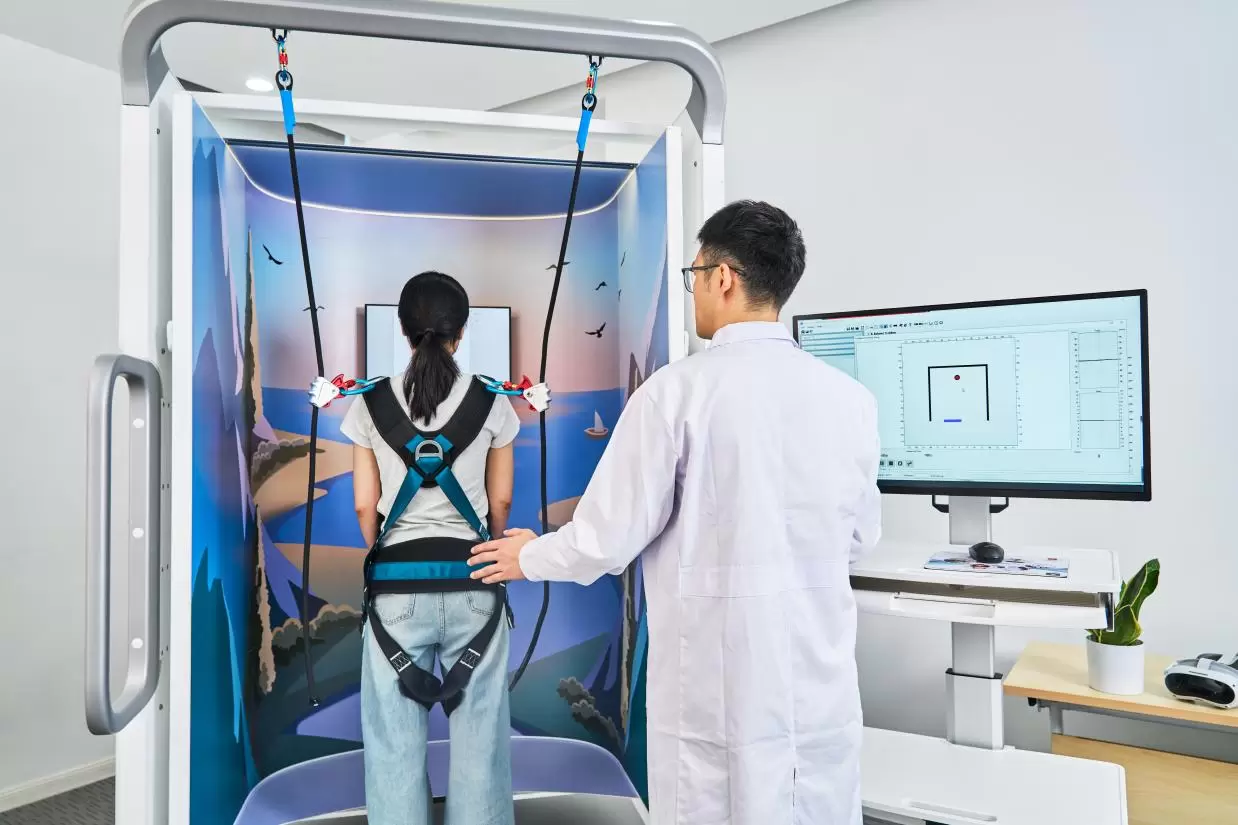
1.Patient Preparation
The patient stands on the force platform wearing a safety harness to prevent falls during testing. Foot placement is standardized to ensure consistent measurement conditions.
2.Test Protocol Selection
The clinician selects the appropriate protocol, such as the Sensory Organization Test, Motor Control Test, or Adaptation Test, depending on the clinical objective.
3.Balance Tasks
The patient is asked to remain as stable as possible while the system introduces controlled changes in the visual environment or support surface. These perturbations challenge how the patient integrates sensory information.
4.Data Acquisition
The force platform records postural sway, weight distribution, and center-of-pressure movement. In motor response tests, the system also captures the timing and symmetry of automatic postural reactions.
5.Software Analysis and Clinical Interpretation
The system generates quantitative scores and comparisons with normative data. Clinicians then interpret the results together with the patient’s history, physical examination, and other vestibular or neurological tests.
A complete CDP balance evaluation often takes about 20 to 30 minutes, although timing can vary depending on the protocol and the patient’s tolerance.
Clinical Applications of Computerized Dynamic Posturography
CDP is widely used in clinical practice to evaluate balance disorders and guide rehabilitation strategies.
Evaluation of Vestibular Disorders
CDP helps clinicians identify whether balance impairment is primarily due to vestibular dysfunction or other sensory deficits. It is often used alongside vestibular tests such as:
•Video Head-Impulse-Test (vHIT)
•Subjective Visual Vertical / Horizontal
Fall Risk Assessment
Posturography is commonly used to evaluate individuals at risk of falling, including:
•Older adults
•Patients with neurological disorders
•Individuals with mobility or sensory impairments
The objective measurements help quantify postural stability and guide preventive interventions.
Neurological Disease Assessment
Conditions affecting the central nervous system may impair sensory integration and motor control. CDP can assist in evaluating patients with:
•Stroke
•Parkinson’s disease
•Multiple sclerosis
•Traumatic brain injury
Rehabilitation and Therapy Monitoring
CDP is also used to track progress during balance rehabilitation programs. By repeating the assessment over time, clinicians can objectively measure improvements in sensory integration and postural control.
The Role of CDP in Modern Balance Assessment
Advances in balance assessment technology continue to improve the precision of postural evaluation. Computerized Dynamic Posturography remains one of the most comprehensive tools available for evaluating sensory integration and postural stability in clinical balance assessment.
By combining multiple standardized tests with advanced visual environments—including mechanical visual surrounds and VR-based visual stimuli—modern Computerized Dynamic Posturography platforms support both detailed balance assessment and rehabilitation planning.
Conclusion
Computerized Dynamic Posturography (CDP) is an advanced method for evaluating balance and postural control by analyzing how visual, vestibular, and somatosensory systems interact during standing and movement. Through standardized tests such as the Sensory Organization Test, Motor Control Test, and Adaptation Test, CDP provides objective insight into sensory integration and motor responses.
With ongoing technological development—including the integration of immersive visual environments and virtual reality—modern CDP systems continue to expand the possibilities for balance assessment and rehabilitation.